Monthly Archives: April 2014
Non-Allergic Rhinitis
Non-allergic rhinitis is a medical condition that presents with the same symptoms as an allergic rhinitis, but without the allergy as the cause, or any other apparent cause.
Symptoms include a runny nose, sneezing, or a stuffy nose. It’s not a serious medical condition, although certain complications may arise from it, such as sinusitis, obstructive sleep apnea and chronic ear infection. When visiting a allergist, they will first rule out any allergy as the cause of rhinitis in order to come to the diagnosis of non-allergic rhinitis.
Triggers for Non-Allergic Rhinitis
There are several possible triggers for non-allergic rhinitis:
-
Infections – Like a cold or the flu
-
Foods – Especially spicy and hot foods, and alcoholic beverages
-
Irritants in the environment – Such as dust, secondhand smoke, perfumes, as well as some chemicals related to specific occupations
-
Some medications – Such as aspirin, ibuprofen, some antidepressants, and blood pressure medications
-
Stress
-
Changes in hormones – For example, in pregnancy or when taking contraceptive pills.
After coming in contact with the trigger, blood vessels in the lining of the nose expand. This leads to a swelling and inflammation can also occur. Although the symptoms of non-allergic rhinitis can look like symptoms of allergic rhinitis, and some common allergens can be the trigger for non-allergic rhinitis, the two are conditions are different.
In allergic rhinitis, the symptoms are caused by an overreaction of the immune systems, which is not the case with non-allergic rhinitis.
Non-Allergic Rhinitis Symptoms
Non-allergic rhinitis presents with the following symptoms:
-
Stuffy or runny nose
-
Sneezing
-
Postnasal drip – mucus in the throat
The duration of the symptoms of non-allergic rhinitis varies greatly. They can last for an hour or two, or for several days. They can appear and disappear during the year. First symptoms usually develop in early adulthood, although they can also appear before. They are also associated with a number of possible complications, including asthma, obstructive sleep apnea, loss of smell, sinusitis, chronic ear infection, and Eustachian tube dysfunction.
Treatment options include both home remedies and medications prescribed by a allergy doctor:
-
Nasal sprays with saline
-
Antihistamine nasal sprays
-
Corticosteroid nasal sprays
-
Decongestants, both oral and nasal
The first thing that needs to be done is to remove the trigger that caused the rhinitis, if possible. Rinsing the nose with saline will help, and it can also be soothing to the nose lining. Antihistamine and decongestant sprays can reduce swelling and other symptoms, however decongestant sprays shouldn’t be used for more than a few days. If they are used more than a few days, they can actually cause more congestion. Corticosteroid sprays are used when antihistamines and decongestants don’t fully help, and they are good in reducing inflammation.
Contact Dermatitis
Contact dermatitis is a skin condition that appears in two ways: allergic contact dermatitis and irritant contact dermatitis. Allergic contact dermatitis is caused by coming in contact with a specific substance the person is allergic to. Irritant contact dermatitis is caused by coming in contact with common irritants.
These two types of contact dermatitis present different symptoms, but neither of them is life-threatening. They usually clear up in a couple of weeks, although they may come back after another contact with the allergen or irritant.
A break-out of contact dermatitis should be discussed with an allergy doctor to determine the best course of treatment, or determine the allergen in the case of allergic contact dermatitis.
Causes of contact dermatitis
Allergic contact dermatitis is caused when a person’s skin comes into contact with an allergen, including:
-
Some antibiotics
-
Balsam of Peru, a compound used in production of cosmetic products
-
Metals, such as nickel and gold
-
Rubber or latex
-
Certain plants, such as poison ivy and poison oak
Irritant contact dermatitis is the more common of the two. It is caused when a person’s skin comes into contact with an irritant, which can be:
-
An acid
-
Soaps, detergent, or fabric softeners
-
Hair dyes
-
Cement
-
Rubber
-
Pesticide or weed killers
Symptoms of contact dermatitis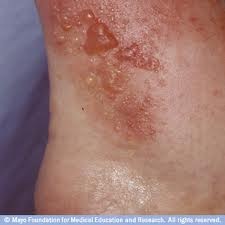
Allergic contact dermatitis symptoms:
-
An itchy rash
-
Blisters
-
Oozing and draining
-
Scaly, raw skin
Irritant contact dermatitis symptoms:
-
Skin redness and a rash
-
Itching, pain and burning
-
Dry and rough skin
The first symptom, which is usually the rash, appears faster in the case of irritant contact dermatitis than in the case of allergic contact dermatitis. The symptoms of allergic contact dermatitis are usually confined to the area that came into contact with the allergen, while symptoms of irritant contact dermatitis tend to spread beyond the contact area. The rash caused by an irritant will tend to be more painful that the one caused by an allergen, and there will also be a burning sensation in the area.
Treatments for contact dermatitis
Treatment options for contact dermatitis include:
-
Topical corticosteroids
-
Oral corticosteroids
-
Oral antihistamines
The first thing that needs to be done in the case of contact dermatitis is to remove the irritant or the allergen. This may include washing the affected area. The mildest cases usually don’t require any other treatment and don’t require a visit to an allergy doctor.
It’s also important to hydrate the skin properly, so moisturizer creams should be used. Topical steroids are used to reduce the inflammation in moderate cases. Steroid creams shouldn’t be used for longer periods of time though, as they may cause the skin to become thinner. Oral corticosteroids are used in more severe cases, and oral antihistamines are used to manage severe itching.
Serving all of New York City and the Tri State Area including Zip Codes: Top Allergist NYC Midtown, Chelsea and Clinton: 10001, 10011, 10018, 10019, 10020, 10036 | Gramercy Park and Murray Hill: 10010, 10016, 10017, 10022 | Greenwich Village and Soho: 10012, 10013, 10014 | Lower Manhattan: 10004, 10005, 10006, 10007, 10038, 10280 | Lower East Side: 10002, 10003, 10009 | Upper East Side: 10021, 10028, 10044, 10128 | Upper West Side: 10023, 10024, 10025
